When the abdominal wall weakens and develops a rip or hole, this condition is known as a ventral or abdominal hernia. Abdominal or intestinal tissue that pushes through the opening and creates a bulge on the exterior of the body is what causes a hernia.
Incisional hernias, which appear at the site of a previous surgery, umbilical hernias, which appear at the navel, epigastric hernias, which appear above the navel, inguinal hernias, which appear in the groin, and femoral hernias, which appear at the upper thigh, are the four most common types of ventral hernias.
A ventral hernia is a type of hernia that occurs when tissue or an organ protrudes through a weakness or tear in the abdominal wall. This can happen for a variety of reasons, including:
- Straining or lifting heavy objects, which can put pressure on the abdominal wall and cause a weakness or tear
- Previous abdominal surgery, which can weaken the abdominal wall and make it more susceptible to herniation
- Congenital defects, which are present at birth and can cause the abdominal wall to be weak or malformed
- Obesity, which can put additional strain on the abdominal wall and increase the risk of herniation
Overall, ventral hernias are typically caused by some form of strain or pressure on the abdominal wall, whether it's due to physical activity, surgery, or underlying medical conditions.
The symptoms of a ventral hernia can vary depending on the size and location of the hernia. Some common symptoms of a ventral hernia include:
- A bulge or swelling in the abdominal area
- Pain or discomfort in the abdominal area, especially when coughing, straining, or lifting heavy objects
- A feeling of fullness or pressure in the abdominal area
- Nausea or vomiting
- Constipation or difficulty passing stool
If you are experiencing any of these symptoms, it's important to see a doctor for a proper diagnosis. They can determine whether you have a ventral hernia and recommend the best course of treatment.
A ventral hernia is typically diagnosed through a physical exam and medical history. During the exam, the doctor will look for signs of a hernia, such as a bulge or swelling in the abdominal area. They may also ask you about your symptoms and any risk factors you may have, such as previous abdominal surgery or a family history of hernias.
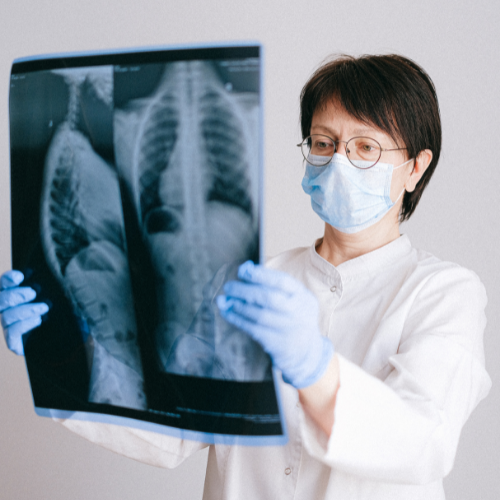
In some cases, the doctor may also order imaging tests, such as an X-ray, CT scan, or MRI, to get a better view of the hernia and its size and location. These tests can help the doctor determine the best course of treatment.
Overall, the diagnosis of a ventral hernia typically involves a combination of a physical exam, medical history, and imaging tests. This will help the doctor confirm the diagnosis and recommend the best course of treatment.
Yes, some ventral hernias can be more serious than others. The severity of a ventral hernia can depend on a few factors, including its size, location, and whether it is incarcerated or strangulated.
An incarcerated hernia is a hernia that becomes trapped in the abdominal wall and cannot be pushed back into place. This can be a serious complication because it can cause the blood supply to the trapped tissue to be cut off, which can lead to tissue death.
A strangulated hernia is a hernia that is both incarcerated and has its blood supply cut off. This is a life-threatening emergency that requires immediate medical attention.
In general, the larger the hernia and the more it affects the blood supply to the trapped tissue, the more serious it is. It's important to see a doctor if you think you may have a hernia, so they can determine the severity and recommend the best course of treatment.
A strangulated hernia is a life-threatening emergency that requires immediate medical attention. Some common symptoms of a strangulated hernia include:
- Severe pain in the abdominal area, which may be constant and severe
- Nausea and vomiting
- Fever
- Redness and swelling in the affected area
- A hard, tender lump in the abdominal area
If you are experiencing these symptoms, it's important to seek medical attention right away. A strangulated hernia can be a serious condition that can lead to tissue death and other complications if it is not treated promptly. A doctor will be able to determine whether you have a strangulated hernia and recommend the best course of treatment.
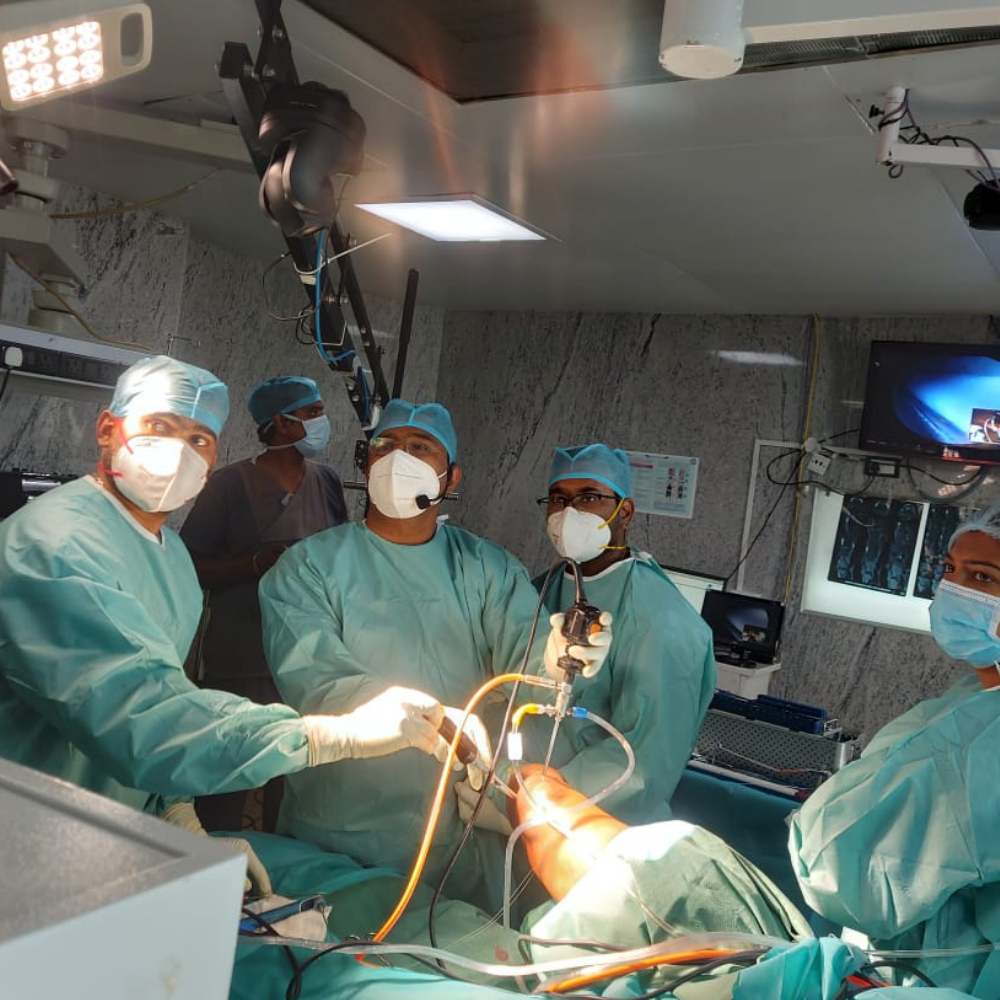
A laparoscopic ventral hernia repair is a minimally invasive surgical procedure used to repair a ventral hernia. During the procedure, the surgeon will make a few small incisions in the abdominal wall and insert a laparoscope, which is a thin, lighted tube with a camera on the end. The laparoscope allows the surgeon to see inside the abdominal cavity and repair the hernia without making a large incision.
The specific steps of the surgery will depend on the type and location of the hernia, as well as the surgeon's preference. In general, the steps may include:
- The patient is given general anaesthesia to put them to sleep and prevent pain during the surgery.
- The surgeon makes a few small incisions in the abdominal wall and inserts the laparoscope.
- The laparoscope is used to view the hernia and any other structures in the abdominal cavity.
- The surgeon may use instruments inserted through the other incisions to push the herniated tissue back into place and repair the weakness or tear in the abdominal wall.
- The incisions are closed and the patient is taken to the recovery room to wake up from the anaesthesia.
Overall, a laparoscopic ventral hernia repair is a minimally invasive surgical procedure that can repair a ventral hernia without the need for a large incision. It is typically done on an outpatient basis, which means the patient can go home the same day as the surgery.
The recovery period after a laparoscopic ventral hernia repair can vary depending on the individual and the extent of the surgery. In general, the recovery period may last for several weeks.
During the first few days after the surgery, the patient may experience some pain, swelling, and discomfort in the abdominal area. The doctor will prescribe pain medication to help manage any discomfort. The patient will also need to avoid straining, lifting heavy objects, and engaging in strenuous activities to allow the incisions to heal.
After the first few days, the pain and swelling should start to improve. The patient will be able to gradually return to their normal activities, although they may need to avoid strenuous activities for several weeks. The doctor will provide specific instructions on when the patient can return to work and other activities.
Overall, the recovery period after a laparoscopic ventral hernia repair is typically several weeks, during which the patient will need to take it easy and avoid strenuous activities. The doctor will provide specific instructions on how to care for the incisions and when the patient can return to their normal activities.
Like any surgical procedure, a laparoscopic ventral hernia repair carries some risks. Some potential risks of the surgery include:
- Infection: The incisions in the abdominal wall can become infected, which can cause fever, redness, swelling, and other symptoms. Placed mesh can get infected and will be removed in that case. Although the risk is lesser than in open surgery.
- Bleeding: There is a risk of bleeding during and after the surgery, which may require a blood transfusion.
- Damage to nearby organs: The laparoscope and other instruments used during the surgery can potentially damage nearby organs, such as the bladder or intestines.
- Adhesions: Scar tissue may form around the repaired hernia, which can cause the intestines to stick together.
- Recurrence: The hernia may come back after the surgery, although this is uncommon.
Overall, the risks of a laparoscopic ventral hernia repair are generally low, but it's important to discuss the potential risks with your doctor before the surgery. They can provide more information and help you make an informed decision about whether the surgery is right for you.